Healthcare is evolving rapidly, and data has become a central driver of better outcomes. Traditional methods often rely on experience and standard protocols, which can overlook subtle trends in patient health. Health data analytics allows providers to extract meaningful insights from vast amounts of information, helping clinicians make more informed decisions. By analyzing patient histories, lab results, and real-time monitoring data, healthcare professionals can predict risks, personalize treatments, and optimize care delivery. Understanding how analytics transforms patient care is essential for both clinicians and administrators who aim to improve efficiency, reduce errors, and enhance overall outcomes.
Understanding Health Data Analytics
Health data analytics is the process of collecting, processing, and analyzing healthcare information to generate actionable insights. This data can come from electronic health records (EHRs), wearable devices, lab tests, imaging, or patient-reported outcomes. The goal is to identify patterns, trends, and anomalies that can guide clinical and operational decisions. Advanced tools, including AI and machine learning, can process complex datasets to uncover insights humans might miss. Analytics turns raw information into strategic knowledge, enabling proactive interventions and personalized patient care.
Predictive Analytics in Healthcare
Predictive analytics allows clinicians to forecast disease progression, identify high-risk patients, and intervene early. For example, patients with chronic conditions like diabetes or hypertension can be monitored continuously. Predictive models analyze past patterns, lifestyle data, and comorbidities to estimate risks. By prioritizing high-risk individuals, healthcare teams can reduce hospitalizations, prevent complications, and allocate resources efficiently. Predictive analytics is not just reactive; it empowers proactive care.
Real-Time Data Monitoring
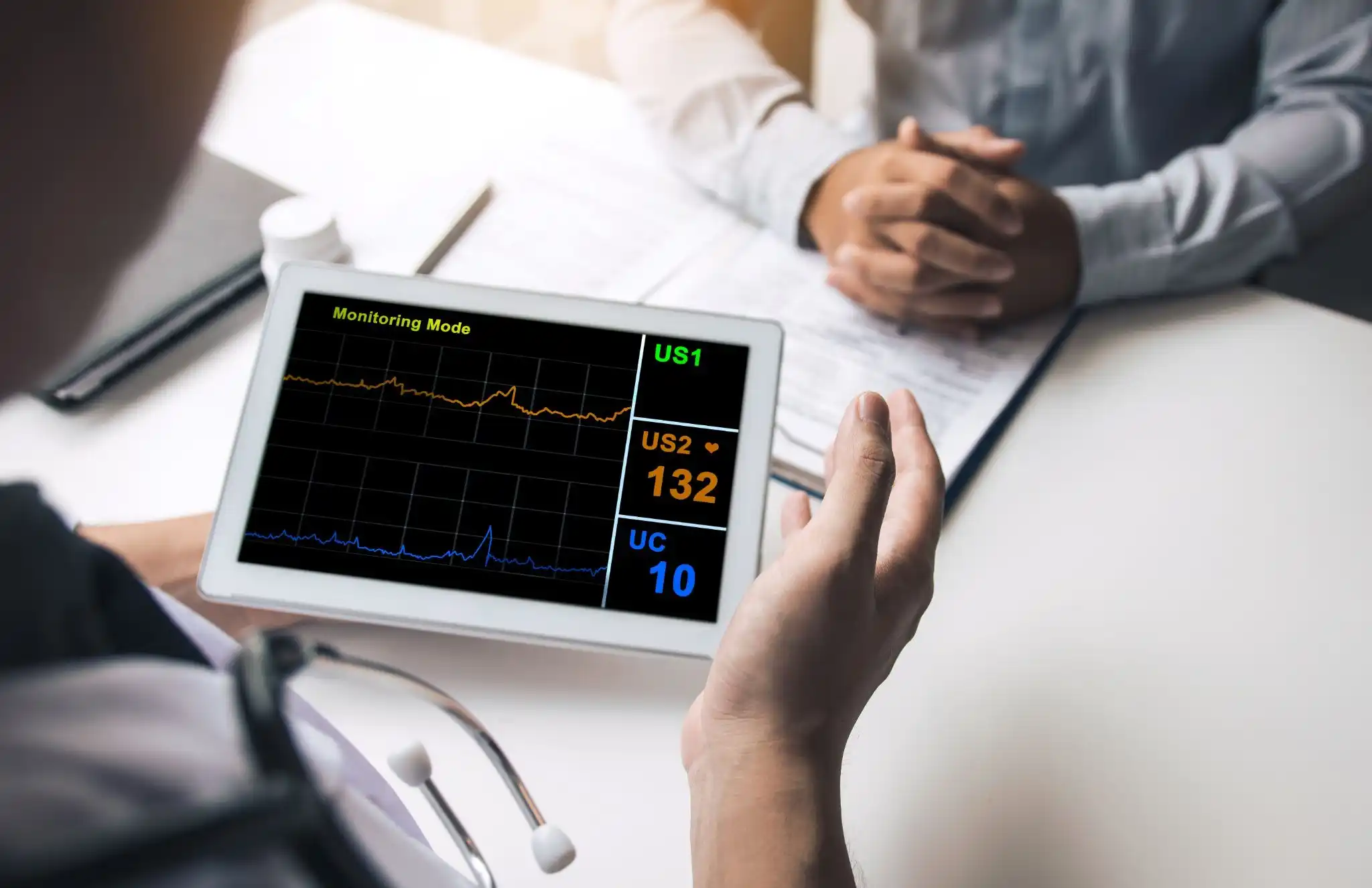
IoT devices and wearable sensors enable continuous monitoring of patient vital signs. Heart rate, oxygen levels, and blood pressure can be tracked in real time, triggering alerts for abnormal values. Real-time data is integrated into hospital systems, allowing immediate response from clinicians. This approach reduces the likelihood of missed warning signs and improves emergency intervention outcomes. Continuous monitoring also supports chronic disease management and post-surgical recovery.
Enhancing Diagnosis Accuracy Through Analytics
Data-driven diagnosis reduces reliance on subjective interpretation. Analytics identifies subtle patterns across large populations, improving the accuracy of tests and imaging results. Machine learning algorithms can flag anomalies in scans or lab results, assisting radiologists and pathologists. By combining historical data with real-time inputs, clinicians can refine diagnoses and reduce errors, leading to faster and more precise care.
Case Example: Oncology
In oncology, health data analytics supports personalized cancer treatment. Patient history, genetic markers, and previous treatment outcomes are analyzed to predict tumor response. Clinicians can tailor therapies for individual patients, maximizing effectiveness while minimizing side effects. Analytics also helps determine the optimal timing for interventions, improving survival rates and quality of life.
Case Example: Cardiovascular Care
Cardiovascular health benefits from integrated data analysis. Continuous monitoring of blood pressure, cholesterol, and heart rate allows early detection of potential complications. Predictive algorithms assess the likelihood of events such as heart attacks, enabling preventative care. This proactive approach reduces hospitalization rates, enhances patient safety, and improves long-term cardiovascular outcomes.
Optimizing Treatment Plans for Better Outcomes
Health data analytics helps create personalized treatment regimens. Patient-specific factors such as age, comorbidities, and lifestyle are considered alongside clinical data. Analytics reduces the trial-and-error approach in therapy selection, ensuring interventions are both effective and efficient. This method improves adherence, reduces side effects, and accelerates recovery.
Personalizing Medication Doses
Medication effectiveness varies among patients. Analytics allows clinicians to determine precise dosing based on metabolism, previous response, and genetic factors. Monitoring patient data during treatment enables timely adjustments, preventing under- or overdosing and enhancing therapeutic outcomes.
Improving Rehabilitation and Therapy Plans
Rehabilitation programs benefit from data-driven insights. Tracking patient progress through wearable devices or digital therapy logs helps clinicians adjust intensity and duration. Personalized plans improve recovery times, ensure adherence, and enhance overall satisfaction with care.
Reducing Medical Errors and Enhancing Safety
Medical errors remain a critical concern. Analytics can identify risk patterns, such as frequent medication errors or lab result inconsistencies. By flagging anomalies early, clinicians can prevent adverse events. Data-driven safety protocols improve patient trust and reduce costs associated with complications.
Implementing Decision Support Systems
Decision support systems integrate analytics into clinical workflows. These tools provide alerts for potential drug interactions, allergies, and abnormal lab results. Clinicians receive guidance that complements their expertise, reducing errors and improving patient safety.
Risk Stratification
Analytics categorizes patients based on risk factors. High-risk individuals receive prioritized attention, ensuring timely interventions. Hospitals can allocate staff, ICU beds, and resources efficiently, preventing complications and improving outcomes.
Improving Hospital and Operational Efficiency
Beyond clinical applications, analytics enhances operational performance. Patient flow, staff scheduling, and resource allocation can all be optimized using historical and predictive data. Efficient operations reduce wait times, improve satisfaction, and enable hospitals to serve more patients without compromising quality.
Patient Flow Analytics
Tracking patient movement through departments identifies bottlenecks and delays. Analytics helps redesign workflows, minimize overcrowding, and streamline admissions and discharges. This approach improves both patient experience and staff productivity.
Supply Chain and Inventory Management
Predictive analytics ensures critical medical supplies and medications are available when needed. Hospitals can anticipate demand, reduce shortages, and manage inventory costs effectively. Optimized supply chains also prevent treatment delays and improve overall care quality.
Population Health Management
Aggregated data provides insights beyond individual patients. Patterns in disease incidence, vaccination coverage, and chronic conditions can inform public health interventions. Analytics helps design targeted community programs, improving overall population health and reducing long-term healthcare costs.
Chronic Disease Monitoring
Regional trends in diabetes, hypertension, and asthma can be identified through data analytics. Health systems can implement preventive measures and tailor interventions for high-risk populations. This proactive approach reduces hospitalizations and improves life quality.
Preventive Healthcare Planning
Data-driven planning supports vaccination campaigns, screenings, and lifestyle interventions. Predictive models highlight gaps in care coverage and help public health authorities allocate resources effectively, maximizing impact and efficiency.
Challenges in Implementing Health Data Analytics
Despite its advantages, analytics faces barriers. Privacy and security of patient data are critical concerns. Interoperability between diverse health IT systems can hinder data integration. Clinicians may resist adopting new tools, and improper use of analytics can lead to inaccurate conclusions.
Ethical Considerations
Patient consent and transparency in data usage are essential. Algorithms must be designed to prevent bias and ensure equitable care distribution. Ethical frameworks guide responsible adoption and foster trust.
Technical and Organizational Barriers
Healthcare staff require training to interpret data correctly. Integrating analytics with legacy systems can be complex, and insufficient IT infrastructure may limit adoption. Leadership support is crucial for successful implementation.
Future Trends in Health Data Analytics
The future of healthcare will be data-driven. AI and predictive analytics will enable even earlier interventions. Integration with telemedicine and remote monitoring will expand access to care. Wearables and mobile devices will continuously feed data into analytics systems. Precision medicine will become the standard, tailoring treatments to individual patients like never before.
Conclusion
Health data analytics is transforming how healthcare is delivered. From accurate diagnoses and personalized treatments to operational efficiency and population health management, data-driven approaches improve outcomes across the board. Effective implementation requires secure, interoperable systems and trained staff. Organizations that adopt analytics strategically can reduce errors, optimize resources, and deliver higher-quality care. The future of patient-centered healthcare depends on embracing health data analytics as an essential tool for clinicians, administrators, and public health authorities.